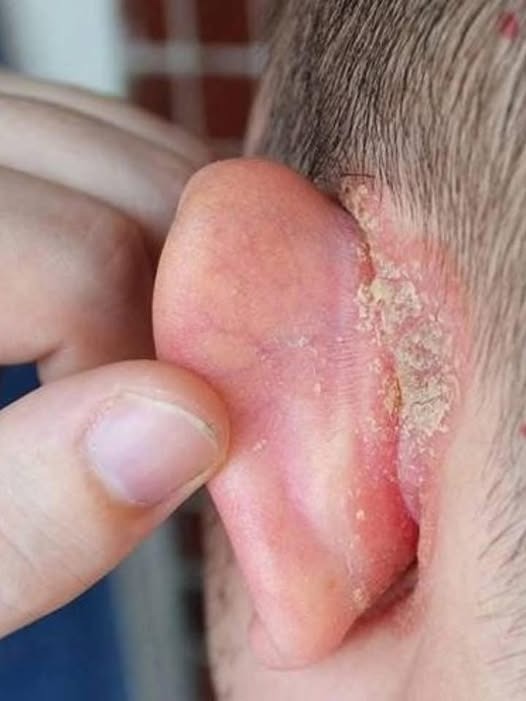
Atopic dermatitis, more commonly known as eczema, is one of the most frequently diagnosed chronic skin conditions in children. It is characterized by inflammation of the skin that leads to redness, dryness, itching, and irritation. Although it can appear anywhere on the body, certain areas are more vulnerable — and the ears are one of them. Because the skin on and around the ears is thin, delicate, and constantly exposed to environmental triggers, it can easily become irritated and inflamed.
Atopic dermatitis is linked to a combination of genetic and environmental factors. Many children who develop it have a family history of eczema, asthma, or seasonal allergies. The condition occurs when the skin barrier does not function properly. Instead of retaining moisture and protecting against irritants, the skin becomes dry and more sensitive. This allows allergens, bacteria, and environmental particles to penetrate more easily, triggering inflammation and intense itching.
The ears are especially susceptible for several reasons. They are exposed to wind, dust, cold air, and sun. Children frequently touch their ears without realizing it, transferring dirt and bacteria from their hands. Hair products such as shampoo, conditioner, and styling sprays may leave residue behind the ears. Earrings, metal studs, hats, headphones, and even mask straps can create friction or introduce allergens that worsen irritation. Because the ear area contains folds and creases, moisture can also get trapped, further aggravating sensitive skin.
Recognizing the signs of atopic dermatitis on your child’s ear early can prevent worsening symptoms. Redness is often the first visible sign. It may begin as a small patch but can gradually spread to the earlobe, behind the ear, or along the outer rim. The skin may appear dry, flaky, or scaly. In some cases, it feels rough or thickened due to repeated scratching — a process known as lichenification. Tiny raised bumps may develop, and the area can look slightly swollen.
Itching is usually the most distressing symptom. Children may rub their ears against pillows, scratch them absentmindedly, or tug at them throughout the day. Younger children may not be able to explain that the sensation is itchy rather than painful, so behavioral clues become important. Increased fussiness, difficulty sleeping, or constant ear touching can signal discomfort.
Parents should also watch for warning signs of infection. When eczema skin becomes cracked from scratching, bacteria can enter. Yellow crusting, oozing fluid, increased warmth, tenderness, or rapid swelling may indicate a secondary bacterial infection. In such cases, prompt medical evaluation is important to prevent complications.
Managing ear eczema typically involves gentle skincare practices. Keeping the area moisturized with fragrance-free creams helps restore the skin barrier. Avoiding harsh soaps, limiting exposure to known triggers, and choosing hypoallergenic products can reduce flare-ups. In some cases, pediatricians may recommend mild topical corticosteroids or other prescribed treatments to calm inflammation.
Understanding that atopic dermatitis commonly affects delicate areas like the ears can help parents respond calmly and effectively. With early recognition and proper care, most children experience significant improvement and better comfort over time.